What Is TMJ Dysfunction?
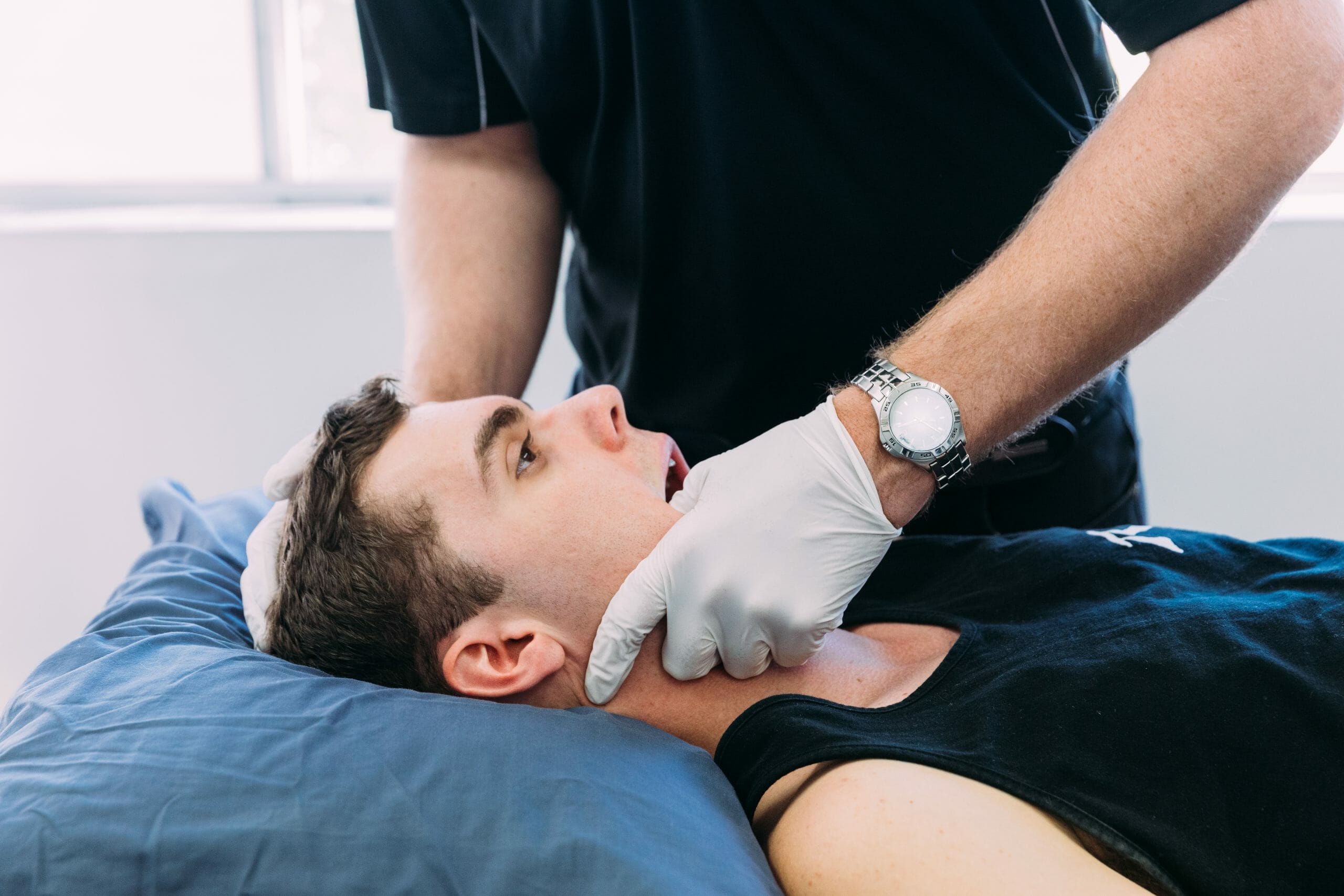
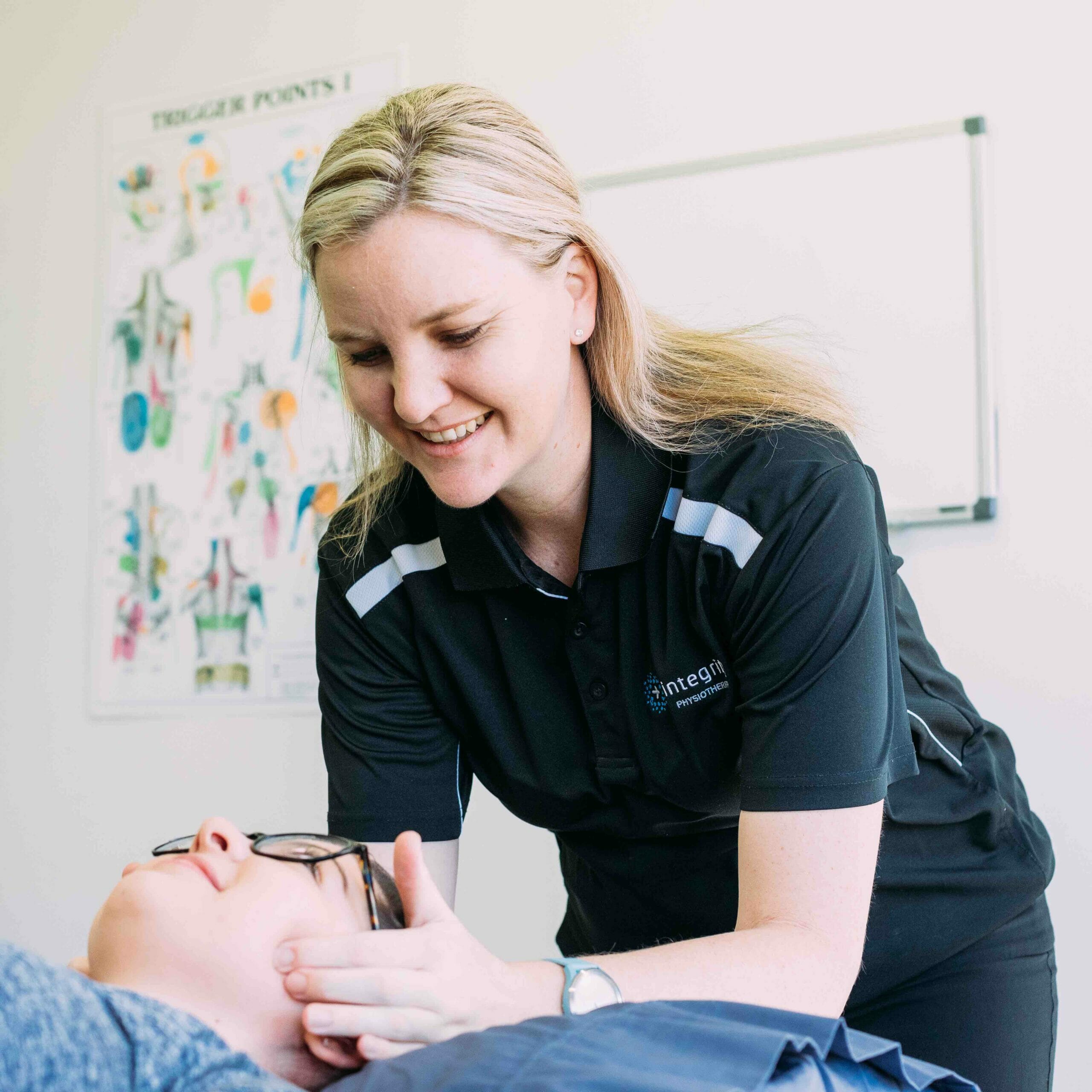
Reduce your pain and jaw stiffness with tailored treatment.The jaw joints or temporomandibular joints (TMJ) are the joints of the located on each side of the face, just below the ears. These joints attach the jaw bone to the base of your skull and are involved in many functions including chewing, speaking, facial expressions and yawning.
The TMJ is one of the most used joints in the body. When there is a problem with the TMJ it is known as a temporomandibular disorder (TMD).
Jaw pain, or TMD, can make everyday life difficult. Find out more about TMD and how jaw pain physiotherapy can help. For more information about jaw pain and the treatment options available, seek advice from your physical therapist experienced in jaw dysfunction (TMD). They will help you understand the cause of your symptoms and the treatment options best suited to your condition.
The most common symptoms people experience when they have TMD is jaw pain, joint noises (crepitus) and difficulty opening the mouth. TMD can also be associated with the neck, teeth, base of the skull and the inner ear. As a result patients often also experience ear pain, temple pain, jaw headaches and upper neck pain. Other symptoms also include:
- Clicking, clunking or locking of the jaw joint
- Pressure or tension in the cheek or face
- Difficulty chewing firm foods
- A blocked feeling in the ear or tinnitus (ear ringing)
The most common causes of jaw pain and dysfunction are related to stress, strain from eating firm or chewy foods, mechanical trauma to the face or dental problems. Some people suffering from TMD have trouble with clenching and grinding, but this is not always the case. Some of the other common causes include:
- Poor bite, underbite/overbite
- Masticatory (chewing) muscle dysfunction
- Jaw joint instability
- TMJ articular disc displacement Arthritis
Some other factors that may contribute to TMD include:
- Poor posture
- Teeth removal
- Dental procedures
- Whiplash
- Neck dysfunction
- Neuropsychological factors
Problems with the temporomandibular joints can be diagnosed by your jaw physiotherapist, dental practitioner or oral medicine specialist. You may be referred for an x-ray, MRI or CT scan for further investigation.
Depending on the severity, acute TMJ disorders may go away without treatment. However, if the symptoms persist jaw physiotherapy can help. In conjunction with jaw physio treatment your GP may need to be involved to assist with pain relief medication, anti-inflammatories or muscle relaxants.
Physio can be a very effective way to treat jaw pain and TMJ disorders. TMJ physiotherapy treatment for jaw pain can identify joint stiffness, muscle tension and movement restriction and provide manual treatment to ease symptoms and return the jaw to its normal function.
Management of your condition by a physiotherapist will include a thorough examination to assess your jaw range of motion, movement patterns and muscle tension. Your physio will determine if the problem is an opening or closing issue.
TMJ opening problem.This is often due to joint stiffness, arthritis, muscle disorders, TMJ disc displacement, postural dysfunction or neck stiffness.
TMJ closing problem.This is often caused by occlusion problems, muscle control problems or joint instability/hypermobility.
TMJ opening disorders are often treated successfully with movement techniques such as dry needling, massage, joint mobilisation and correction of any relevant neck involvement. TMJ closing disorders may involve a combination of dental and physiotherapy involvement including splinting and exercise prescription.
Understanding Jaw Pain & TMJ Disorders
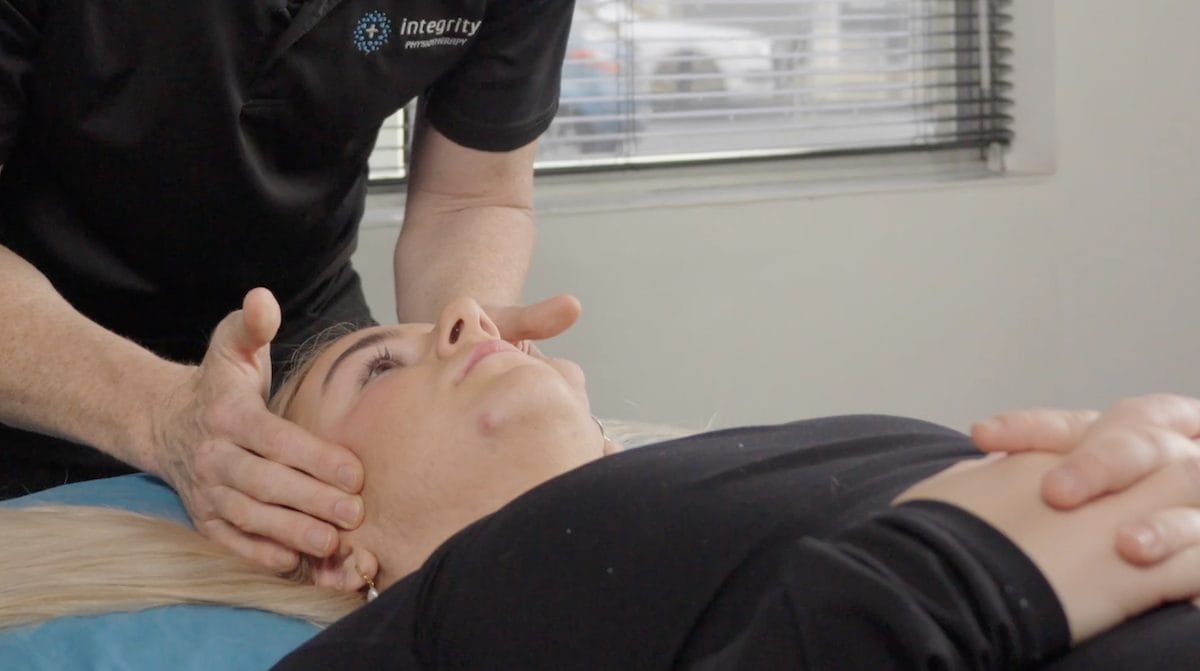

Everything you need to know about physiotherapy for jaw pain and TMJ disorders.
- Jaw pain or tightness
- Clicking, popping or grinding sounds in the jaw
- Difficulty opening or closing the mouth
- Facial pain or headaches
- Ear pain, pressure or ringing
- Neck or shoulder tension
- Teeth grinding or jaw clenching (bruxism)
- Stress and muscle tension
- Poor posture, especially forward head posture
- Trauma or injury to the jaw or neck
- Dental or bite-related issues
- Prolonged chewing or hard foods
- Manual therapy to the jaw, neck and surrounding muscles
- Jaw and postural exercises
- Muscle relaxation and load management strategies
- Education on habits that aggravate TMJ pain
- Techniques such as dry needling (where appropriate)
- Chronic Pain Sufferers: If your back pain has been ongoing, we take a steady, supportive approach, focusing on pain relief, improving movement, and helping you manage flare-ups with confidence.
- Athletes: Whether you're training, competing, or recovering from an injury, we provide sport-specific physiotherapy to reduce pain, restore performance, and prevent recurrence.
- Post-Surgical Patients: After back surgery or procedures involving the spine, we offer guided rehabilitation to rebuild strength safely, reduce stiffness, and support a smooth recovery.
- Pregnant and Postnatal Women: We help manage lower back and pelvic pain during pregnancy and support postnatal recovery with gentle, targeted treatment and core reactivation strategies.
- Older Adults: We provide safe, hands-on care to improve mobility, reduce stiffness, and help you stay active and independent, with a focus on balance, strength, and fall prevention.
- Jaw pain lasts longer than a few days
- Your jaw clicks, locks or feels unstable
- Pain affects chewing, speaking or sleeping
- Headaches or ear symptoms persist without explanation
- Early treatment can prevent TMJ issues from becoming chronic.